How Well it Works
In the study presented below, four graphs show how 92 people were able to reduce their nighttime teeth clenching using the SleepGuard biofeedback headband. Each graph is a graph of how one quarter of the group did. The first graph is an average of the people who did the best. The second graph is the average of the group that did the second best. The last graph is the average of the people who had the most challenges.
 How the SleepGuard Headband is WornThe SleepGuard biofeedback headband is worn on the head during sleep, as shown in this photo. |
The most responsive 25% of people
The averaged results from the most responsive 25% of the 92-person test group is shown first and the least responsive 25% of the people are averaged in the last graph below. Average nightly reduction in bruxism time was measured as the difference between the normalized average nightly clenching time during the three days of initial baseline measurement (this average was normalized to 1 for all patients), and the normalized average nightly clenching time during the last three days of the 30-day study.
The average from the most responsive 25% of the people are shown in figure 2 below.
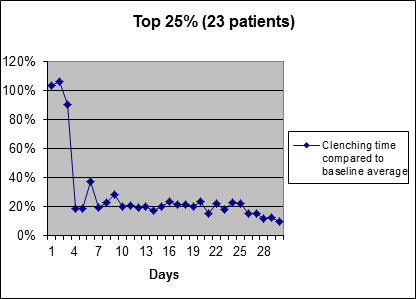 The most responsive 25%Average clenching time reduction of most responsive 25% of users during first 30 days of use of SleepGuard headband (biofeedback starts on 4th day).
|
The people in the group above showed an average initial reduction in bruxism time of 80% in just one day after turning on the biofeedback, and by the end of the month they had a nightly bruxism time reduction of 90%. Since clenching force typically ramps up during a clench, cutting the clench short cuts out the most damaging part of the clench.
The the reduction in nightly clenching time for the next best performing 25% of participants (23 people) is shown below.
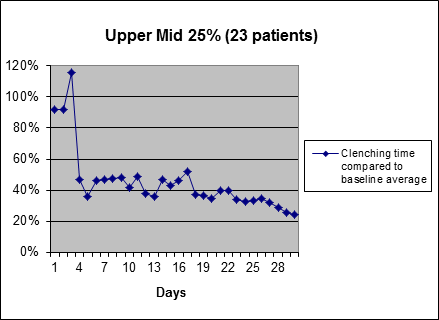 The second most responsive 25%Average clenching time reduction of the second most responsive 25% of users during first 30 days of use of SleepGuard headband (biofeedback starts on 4th day). |
The “remaining bruxism” of these people at the end of the month is about twice that of the most responsive group (in terms of remaining clenching time), but still very low. Again, because the damaging, higher-force later part of each clench is not happening, the pain is reduced far more than one might think from the percentage reduction in clenching time indicated above.
In both of the groups above, nightly clenching time was trending down steadily toward the end of the month, indicating that these people are on the average training themselves out of their bruxism habit. This is supported by statements people made in follow-up interviews several months later, where many people said that after using the SleepGuard headband for between two and four months, they were able to go for long periods (over a month) without using the headband before any daily pain returned.
Most people in the second group, like the first group, reported substantial reduction or complete elimination of pain such as jaw pain, migraines, TMJ pain, etc..
The average of the data from the next most responsive 25% (23 people) is shown below.
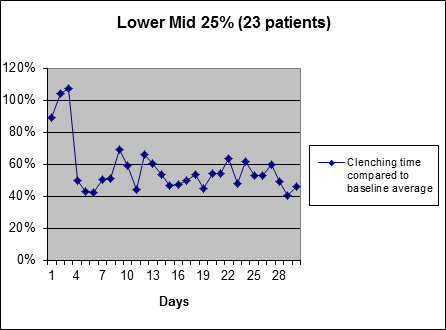 The third most responsive 25%Average clenching time reduction of third most responsive 25% of people during first 30 days of use of SleepGuard headband (biofeedback starts on 4th day). |
These people experience approximately a 60% initial reduction in nightly clenching time when the biofeedback is turned on, and their nightly clenching times remain at roughly this level for the rest of the month. In addition to the reduction in clenching time, it is estimated that this group experiences a reduction in force while clenching of about 50%.
There is no obvious trending downward toward the end of the month for the above group, so they may not be training themselves out of their bruxism habit, but continued use of the biofeedback helped to keep them out of pain and prevent ongoing damage from nighttime clenching. Some people in this group reported a complete elimination of pain symptoms, including TMJ pain and migraines.
The data from the least responsive 25% of people is shown in figure 6 below.
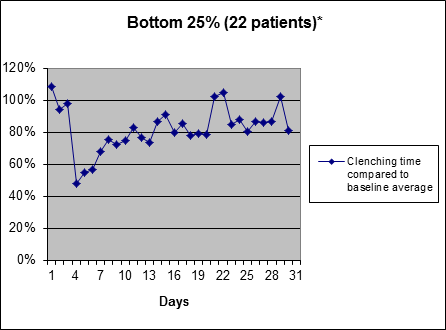 The least responsive 25%Clenching time reduction of least responsive 25% of people during first 30 days of use (biofeedback starts on 4th day). |
These people respond well to the biofeedback at first, and then over time, their nightly bruxism times came back to a level close to their baseline levels.
One way to interpret why this may happen is that each person may be thought of as being of “two minds”. One part of the mind wants to learn to relax and get out of the bruxism habit. This part of the mind hears the biofeedback tone as a caring reminder about something important. The other part of the mind wants to learn to ignore any sound heard during sleep, and continue with any addictive behavior. For this group, this second part of the mind appears to win out, and patients return to near-baseline levels of clenching (though there is some reduction in clenching time and some reduction in clenching force, so many people in this group still had a significant reduction in pain).
The Importance of Daytime Response Conditioning
In the study presented above, written instructions directed all participants to spend at least a few minutes per day in the first few days doing “response training” to train a part of their subconscious mind to cooperatively and immediately relax jaw muscles when the RelaxTone biofeedback sound was heard. The instructions explained that the intent was for this training to carry over into sleep, and increase the ability to respond (by relaxing jaw muscles) in sleep without waking when the biofeedback tone is heard.
It was found at the end of the study that many of the people whose results put them in the least responsive group above had not continued their daytime practice past the first few days. This shows that it can be important to keep up the daily practice to keep training the part of the subconscious mind that will be relied on to relax jaw muscles during sleep whenever the gentle RelaxTone biofeedback sound is heard.
Mental Alignment With the Biofeedback Process
Mental alignment with the process has been found to be one of the key factors influencing how well people will be able to respond during sleep. Users who describe themselves as feeling grateful for the audio reminder to relax their jaw muscles, tend to decrease their nighttime clenching faster and by a higher percentage than users who do not describe themselves as feeling grateful for the reminder.
Conclusion
This study showed that about 75% of people are able to reduce their nightly clenching substantially through ongoing use of the SleepGuard biofeedback headband in its standard configuration. On the average, most of the benefit in nightly clenching time reduction is realized from the day the biofeedback is turned on. Reduction in pain or elimination of pain usually follows, starting within several days. About 25% of people appear to remain at the initially-reduced level as they continue use, and there are indications that about 50% of people are able to continue to steadily reduce their nightly clenching times beyond the initial reduction.
